How Chronic Pain Affects Your Heart
Chronic pain is the single most common major medical issue among adults. In the U.S. alone, chronic pain is estimated to affect over 50 million adults and cost $635 billion annually, more than the annual costs of heart disease, cancer, and diabetes combined.
And while the primary symptoms of chronic pain are clear, such as persistent, sometimes debilitating pain across different parts of the body, there are less obvious side-effects as well. In this article, we reveal how chronic pain can play a significant role in the development of serious heart conditions.

Perhaps it should come as no surprise then that the second most common medical issue among US adults is… you guessed it, heart disease. Heart disease affects over 20 million people and costs an estimated $219 billion each year. Do you want to guess what the #1 most common medical condition is? If you guessed chronic pain, you are correct. So it should come as no surprise that the two often occur together.
Now, suffering from chronic pain does not automatically mean you will develop heart problems. But there is a very real connection between the two, and it’s important for chronic pain patients to understand how it works so they can properly manage it.
KEY TAKEAWAYS
- Chronic pain can stimulate the autonomic nervous system and trigger a persistent “fight-or-flight” response, leading to elevated heart rate and blood pressure — placing extra strain on the heart.
- Because chronic pain often limits physical activity, disturbs sleep, and is linked with anxiety or depression, these indirect lifestyle effects can contribute to elevated cholesterol and increased risk of cardiovascular disease.
- Managing or treating chronic pain isn’t just about relief of symptoms—it can also be important for protecting heart health, since reducing pain may lower the long-term risk of serious cardiac issues.
Table of Contents
- How chronic pain affects blood pressure and heart rate
- Chronic pain and high cholesterol
- How to prevent heart conditions caused by chronic pain
How chronic pain affects blood pressure and heart rate
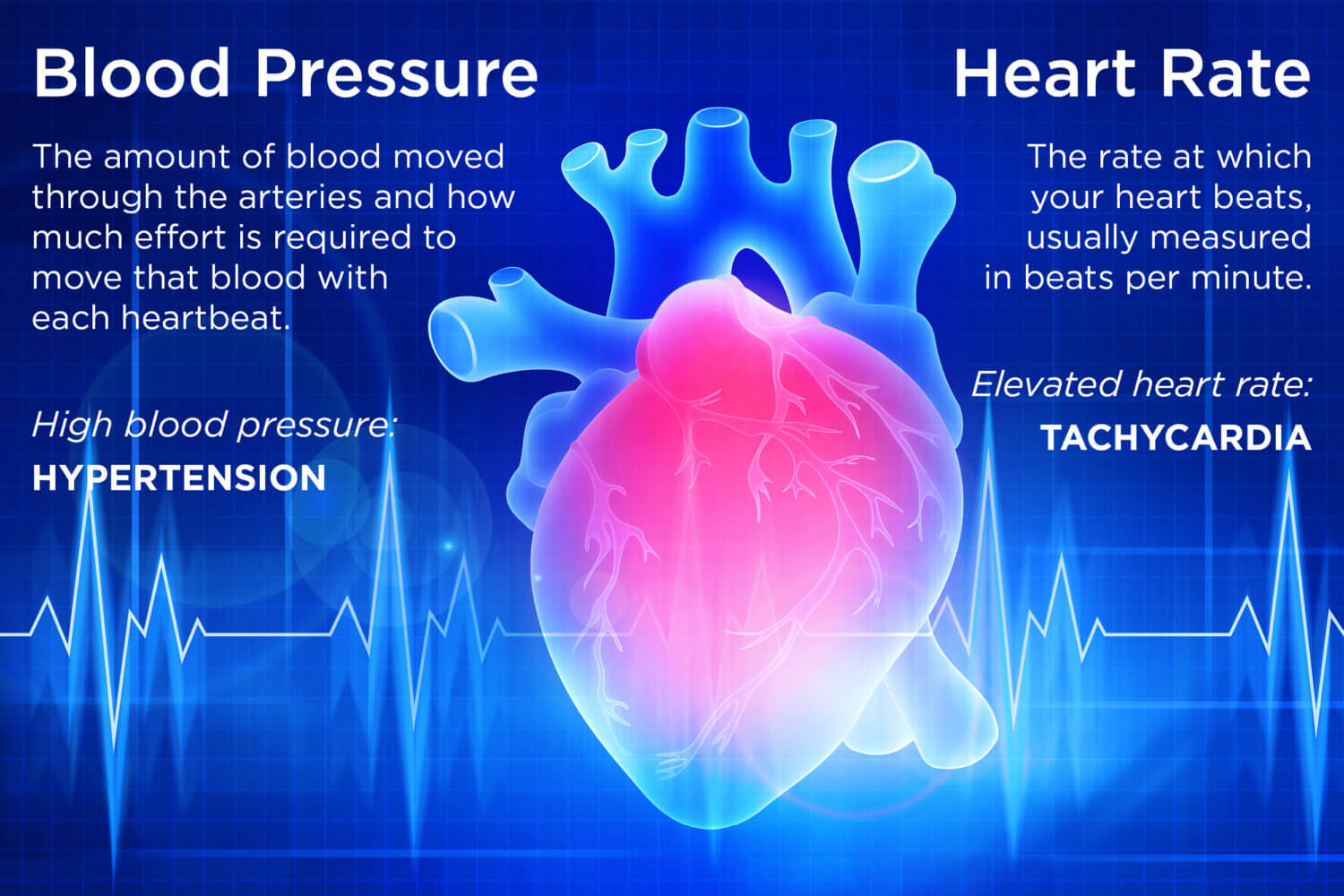
Among the most common cardiovascular conditions are high blood pressure (hypertension) and increased heart rate (tachycardia). Hypertension alone affects over 3 million Americans each year.
But let’s begin by pointing out that these conditions are not always cause for concern. Your blood pressure and heart rate regularly rise (temporarily) due to things like stress or strenuous physical activity. The latter is in fact GOOD for your heart health. The trouble starts when blood pressure and heart rate are continuously elevated.
Blood pressure is determined by the amount of blood moved through the arteries and how much effort is required to move that blood with each heartbeat. Heart rate is determined by how fast your heart beats, usually measured in beats per minute.
Both hypertension and tachycardia force the heart to work harder to move blood throughout the body. The longer the heart is overworked, the greater the risk of heart failure, heart attack, or other serious health problems like stroke.
So where does chronic pain come into play in all this? Experts believe there are two primary reasons that chronic pain causes hypertension and tachycardia.
Pain has shown to stimulate the autonomic nervous system.
The autonomic nervous system is responsible for all the involuntary actions your body performs, such as breathing, sweating, digestion, and, you guessed it, heart rate and blood pressure. When this system becomes stimulated by pain signals, heart rate and blood pressure increase.
Your brain responds to pain signals by launching your body’s flight-or-flight response.
The flight-or-flight response is a reaction to stressful or dangerous situations. When activated, fight-or-flight stimulates the release of hormones such as adrenaline. These hormones cause your heart to pump harder and faster so your blood can deliver oxygen to where it is needed most.
When you suffer from chronic pain, your system is constantly being bombarded by pain signals. When this is happening, your body’s natural reactions can put excessive stress on your heart and may result in serious cardiac health issues.
Chronic pain and high cholesterol
High cholesterol is a major contributor to heart issues and affects millions of Americans every year.
Blood cholesterol is a waxy, fat-like substance made by your liver. Your body needs it to perform important jobs, such as making hormones and digesting fatty foods.
The body makes enough cholesterol all on its own, so when excess cholesterol is introduced via health conditions like type 2 diabetes or obesity, or lifestyle factors like an unhealthy diet, smoking, excessive alcohol consumption, and lack of activity, it causes a buildup of fat deposits called “plaque.”
This plaque buildup concentrates on the walls of your arteries. Over time, this causes the insides of your arteries to narrow, blocking blood flow to vital organs and body parts. This decreased blood flow can increase the risk of heart attacks and heart disease.
Enter chronic pain once again. Unlike in the case of hypertension and tachycardia, chronic pain does not stimulate a natural bodily response that increases cholesterol levels. Chronic pain’s role is more indirect, specifically how it influences lifestyle factors that can result in elevated cholesterol. Some of the most common and impactful factors include:
Lack of activity
One of the best ways to prevent high cholesterol levels is regular exercise and physical activity. Exercise stimulates the release of enzymes that help remove bad cholesterol from the blood. However, those who suffer from chronic pain tend to be less active due to the limitations of their condition. As a result, the body won’t be able to remove bad cholesterol as effectively, allowing plaque to build up more rapidly.
Lack of sleep
Sleep is when your body, including your heart, recharges. Your blood pressure drops, your heart rate slows, and your breathing relaxes, allowing your heart to recover from the day. But sleep can be difficult to come by when you have chronic pain. Studies have shown that lack of sleep can result in your heart not getting the rest and recovery it needs. Studies have shown that lack of sleep can lead to higher levels of bad cholesterol in the blood stream.
Anxiety and depression
Chronic pain has a tendency to significantly limit your ability to do many of the things you love. This is a reason that many chronic pain sufferers develop depression. Studies have shown that depression can cause stress hormones to be consistently elevated, which in turn can cause high cholesterol levels. Additionally, anxiety and depression can result in increased food consumption, fat storage, and weight gain, often called “stress eating,” which can also cause high cholesterol.
Additionally, each one of these factors has the potential to cause or exacerbate the others. For example, depression may make it more difficult for you to commit to an exercise routine while also keeping you awake at night as you focus on your worries. This can collectively result in a frightening cycle that accelerates the onset of serious heart problems.
That is why it is so important to be aware of these risks and take steps to manage them.
How to prevent heart conditions caused by chronic pain
As they say, “an ounce of prevention is worth a pound of cure.” And as with many health conditions, one of the best ways to prevent heart problems if you have chronic pain is by making smart, healthy lifestyle choices.
Try to get in at least 30 minutes of exercise or physical activity each day.
It can be anything from a complete workout regimen to simply taking a nice long walk. Regular activity is one of the best things you can do for heart health and overall wellbeing, and it can go a long way in preventing a lot of other issues that contribute to heart conditions. But make sure you speak to your doctor before starting any kind of exercise routine, just to make sure you are making appropriate choices that won’t worsen your pain or cause further complications.
Get quality sleep.
This can be difficult when you have chronic pain, but it is essential. As we previously mentioned, sleep is when your body recovers. If you do not get good sleep, your pain will likely only get worse, making it more likely that serious complications could develop. Talk to your doctor about safe options to help you get a good night’s rest.
If you ever feel unusually anxious or worried that you may be depressed, do not ignore those feelings.
Especially if you already suffer from chronic pain. Instead, discuss your concerns with a licensed mental health professional. Best case scenario, you can have peace of mind. But if there is something deeper going on, you will have established a relationship with someone who can help you through it.
FAQs
Yes. Chronic pain activates the body’s stress response, which can raise blood pressure and heart rate over time. This constant strain on the cardiovascular system may increase the risk of heart disease or other cardiac complications.
Pain triggers the release of stress hormones like cortisol and adrenaline. These hormones cause your heart to work harder to deliver oxygen where it is needed, increasing blood pressure. While this is common in short bursts, such as during exercise, persistent elevated heart rate can overwork your heart to the point of failure.
Healthy lifestyle habits—such as regular, pain-appropriate physical activity, improved sleep quality, stress management, and addressing emotional health—can significantly reduce cardiovascular strain. Combining these with medical pain management may lower your long-term risk of heart complications.
Absolutely. Treating and managing chronic pain through medical interventions, physical therapy, or stress-reduction strategies can reduce chronic stress on the cardiovascular system. Lower stress hormone levels and increased activity capacity help stabilize blood pressure and support better heart health.
If persistent chronic pain is accompanied by high blood pressure, rapid heart rate, shortness of breath, chest discomfort, or unusual fatigue, discuss these symptoms with a healthcare provider. Early evaluation and management may help reduce both pain and cardiovascular risk.
Get to the Heart of the Issue at Twin Cities Pain Clinic
Along with the helpful prevention tips we have reviewed, it is important to get right to the heart of the problem. If you suffer from chronic pain, get it treated. Chronic pain is tough, but it’s not so tough that you have to let it beat you.
Luckily, chronic pain management is a rapidly advancing field and today there are a wide variety of innovative and effective treatment options that can provide significant pain relief. By reducing, or perhaps even eliminating, your chronic pain through treatment, you may be able to tremendously lessen the possibility of developing serious heart conditions.
A reputable pain management provider, like Twin Cities Pain Clinic, can help identify the root cause of your pain and prescribe an appropriate treatment plan. By taking steps to get your pain under control, you will be doing your body, and especially your heart, a big favor.
If you suffer from chronic pain and want to speak with one of our pain experts, click here to get started.
DISCLAIMER
The contents of this article are intended for informational and educational purposes only and are not intended as a substitute for professional medical advice, diagnosis or treatment. Always consult with a physician or other qualified healthcare provider before engaging in any action or decision-making based on the content of this article. Never disregard or delay seeking professional medical advice or treatment because of the content of this article or any other content on the Twin Cities Pain Clinic website. Reliance on any information conveyed on the Twin Cities Pain Clinic website without direct consultation with a healthcare professional is solely at your own risk.
Sources
- Bernstein, Susan. “Stress and High Cholesterol: What’s the Link?” WebMD, www.webmd.com/cholesterol-management/stress-cholesterol-link
- “Can Chronic Pain Increase Bad Cholesterol (LDL)?” AnxietyCentre.com, www.anxietycentre.com/faq/can-chronic-pain-increase-bad-cholesterol-ldl/#:~:text=The%20combination%20of%20anxiety%2C%20chronic
- CDC. “About High Blood Cholesterol.” Centers for Disease Control and Prevention, 6 Feb. 2019, www.cdc.gov/cholesterol/about.htm
- —. “Chronic Diseases in America.” Cdc.gov, 2022, www.cdc.gov/chronicdisease/resources/infographic/chronic-diseases.htm
- —. “Health Topics – Heart Disease – POLARIS.” Centers for Disease Control and Prevention, 17 Aug. 2021, www.cdc.gov/policy/polaris/healthtopics/heartdisease/index.html#:~:text=Economic%20Burden
- Charkoudian, Nisha, and Jennifer A. Rabbitts. “Sympathetic Neural Mechanisms in Human Cardiovascular Health and Disease.” Mayo Clinic Proceedings, vol. 84, no. 9, 1 Sept. 2009, pp. 822–830, pubmed.ncbi.nlm.nih.gov/19720780/#:~:text=The%20sympathetic%20nervous%20system%20plays%20a%20key%20role, 10.1016/S0025-6196(11)60492-8
- “Chronic Pain Linked to Higher Risk of Heart Attack and Stroke.” Harvard Health, 1 Sept. 2020, www.health.harvard.edu/heart-health/chronic-pain-linked-to-higher-risk-of-heart-attack-and-stroke
- Fayaz, Alan, et al. “The Association between Chronic Pain and Cardiac Disease.” The Clinical Journal of Pain, vol. 32, no. 12, Dec. 2016, pp. 1062–1068, 10.1097/ajp.0000000000000359
- Gaskin, Darrell J., and Patrick Richard. “The Economic Costs of Pain in the United States.” The Journal of Pain, vol. 13, no. 8, Aug. 2012, pp. 715–724, 10.1016/j.jpain.2012.03.009
- Mayo Clinic. “High Blood Pressure (Hypertension) – Symptoms and Causes.” Mayo Clinic, 2021, www.mayoclinic.org/diseases-conditions/high-blood-pressure/symptoms-causes/syc-20373410
- —. “Tachycardia – Symptoms and Causes.” Mayo Clinic, www.mayoclinic.org/diseases-conditions/tachycardia/symptoms-causes/syc-20355127#:~:text=Tachycardia%20(tak%2Dih%2DKAHR
- Saccò, Marcella, et al. “The Relationship between Blood Pressure and Pain.” The Journal of Clinical Hypertension, vol. 15, no. 8, 10 June 2013, pp. 600–605, pubmed.ncbi.nlm.nih.gov/23889724/, 10.1111/jch.12145
- Tennant, Forest. “Treat the Pain… Save a Heart.” Practical Pain Management, 2009, www.practicalpainmanagement.com/pain/other/co-morbidities/treat-pain-save-heart
Author Bio